Peri-implantitis is report to affect approximately 7-10% of all implants after 10 years of service. We currently don’t know what the prevalence of peri-implantitis is after 10 years of service.
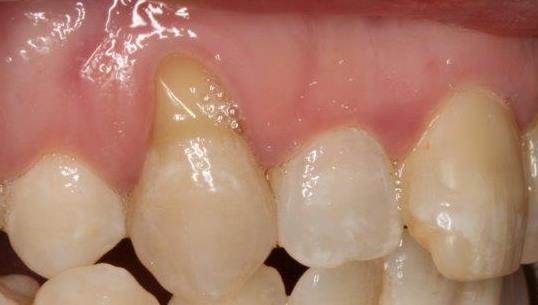
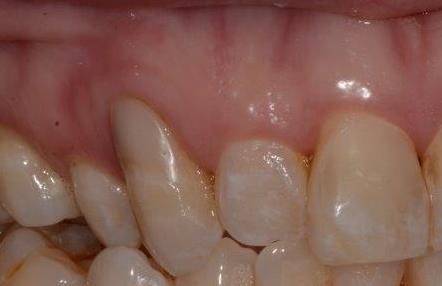
Mrs JN presented complaining of recurrent gum infection around two implants placed about 18 years ago. JN was diagnosed with per-implantitis and went on to have pocket reduction surgery around the implants and implantoplasty due to the non-regenerable defect around the implants. The result was as predicted from this type of treatment:
1-minimal bleeding on probing
2-pocketing reduced from 9mm to 3mm
3-increase in gum recession
4-
The primary measure for success in mucogingival surgery is the percentage of root coverage which is measured from the CEJ. It is important to note that the CEJ migrates coronally with toothwear, and as such, achieving a high level of dentine coverage is not possible in cervical wear patients. In order to optimise the aesthetic outcome and to reconstitute the anatomical dental harmony, restorations may need to be utilised to recreate a new enamel dentine junction. Zuchelli et al 2006 and Cairo et al 2011 demonstrated using the height of the interproximal attachment to predict the post-operative final position of the gingival margin. These predictive formulas are useful guides but are not conclusive because they do not take into account soft tissue type and tooth morphology and positon.
Restorative reconstitution of the CEJ is best undertaken preoperatively with indirect or direct restorations. This will allow for easy polishing and refining the margins and avoids traumatising the gingival margins post-operatively. Definitive restorations should be delayed 6 months post operatively to ensure stability of the gingival margin and successful cessation of any traumatic habits. Referring dentists usually undertake the restorative management of these patients and I often assist by denoting where the gingival margin is likely to be.This is an example of a patient- KP who had two protracted courses of orthodontic treatment with fixed appliances resulting in severe gingival recession which was progressively worsening. Her smile aesthetics were further complicated by a high lip line which clearly displayed the asymmetric gingival aesthetic line. Previous dentists choose to mask the exposed dentine with composite resin rather than gingival tissue which did not improve aesthetics because it failed to address the discrepancy in the gingival margins.
The patient was successfully managed with a de-epithelialised free gingival graft and a coronally advanced flap. The CEJ was reconstituted with composite resin to produce 100% root coverage and an overall harmonious appearance. I would like to Thank Dr Andy Bolam for choosing to refer KP to my care and for correctly noting the progression of her recession. I would also like to thank Juliette Reeves, RDH for the excellent post operative maintenance which optimised the surgical result.