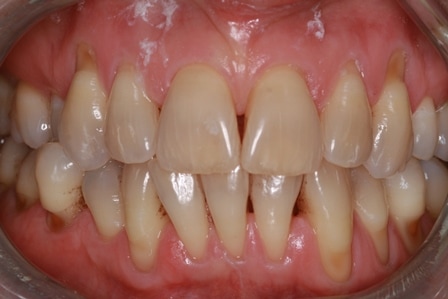
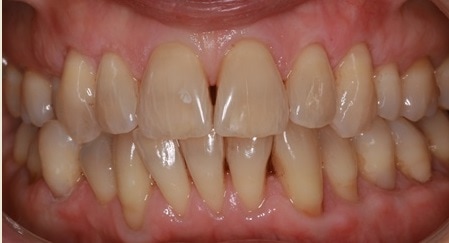
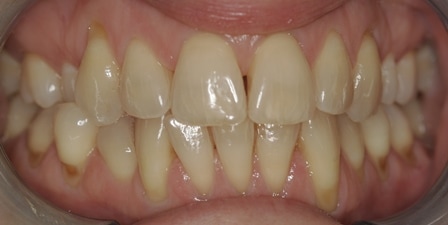
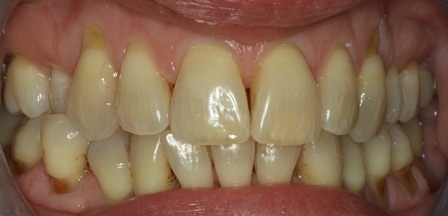
Gum recession so what and who cares?? Relax and keep cleaning it and it will be fine! NOT TRUE ANY MORE!!!!
These statements will soon be a thing of the past. Chambrone et al 2016 demonstrated with systematic review and a meta-analysis that about 80% of untreated recession defects worsened over 24 months moreover the number of recession defects also increased. The odds ratio of this happening is over 2 meaning it is likely to happen.
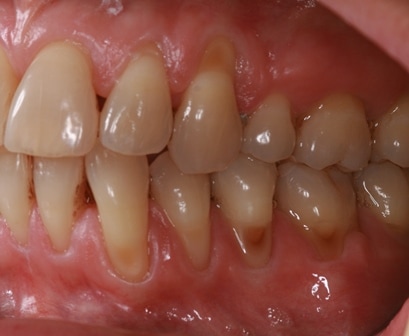
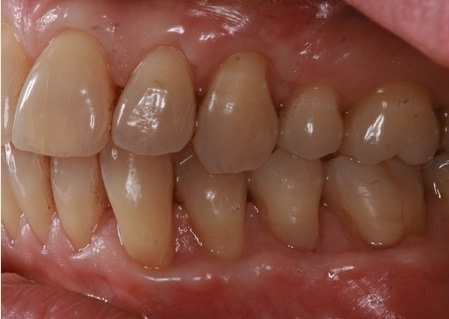
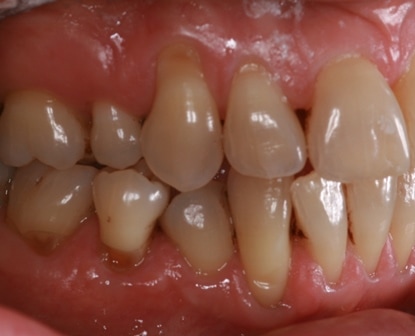
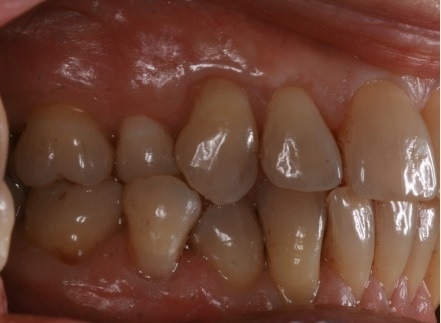
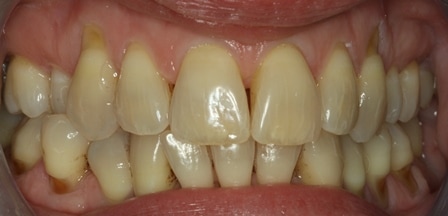
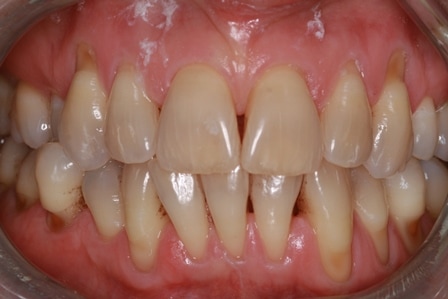
This is problematic for busy general practitioners who use BPE scores a method of monitoring periodontal health. Such a scoring system will not track changes in recession depths. Even conventional charting will not easily detect these changes. Clinical photographs are the best means to monitor and detect changes.
Given the high prevalence of gingival recession and the high likelihood of progression, when should we treat it? The answer is:
- To maintain or improve aesthetics
- Reduce the effects of toothwear
- Reduce sensitivity
- If recession defect reaches the mucogingival junction or exceeds 5mm in depth. These are end points which if exceeded are associated with higher surgical complexity in turn poorer outcomes
What will happen to augmented sites over time? Agudio et al 2016 showed a high degree of stability of the achieved immediate post operative result for over 18 years of follow up.
This patient was carefully and diligently monitored by James Goolnik and Christine at Bowlane Dental. They detected progression in her toothwear and recession. Following referral, I managed her with acellular dermal matrix grafts to reduce the risk factors for progression such as thin phenotype and lack of keratinised tissue. Composite resin restorations were used to restore the CEJ to reduce risk of wear and to obtain 100% root coverage on the uppers and close to 80% root coverage on the lowers despite the Miller II/III defects. Christine Arran provided exemplary post-operative maintenance that facilitated this result and James Goolnik will continue to follow the patient’s progress over time.